Latest Vaccination Guidelines: Protecting Your Health & Community
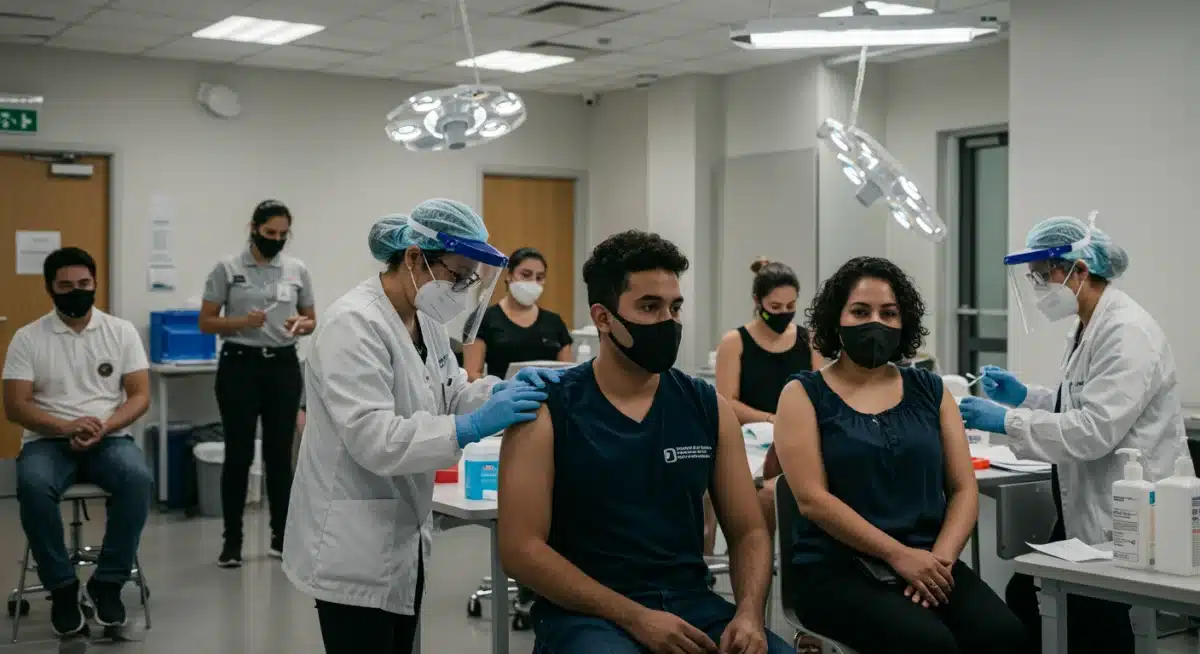
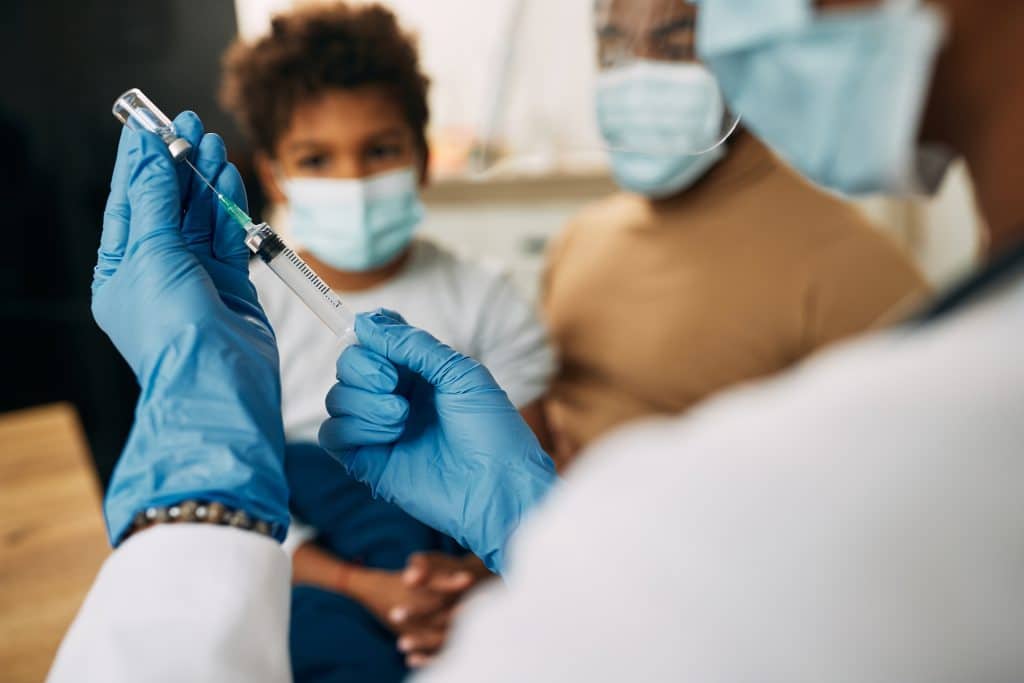
Staying informed about vaccination guidelines USA is more important than ever for personal well-being and public health. These guidelines, regularly updated by leading health organizations, serve as a critical roadmap for protecting ourselves and our communities from infectious diseases.
understanding the importance of vaccination guidelines
Vaccination guidelines are developed by expert committees, such as the Advisory Committee on Immunization Practices (ACIP) in the United States, which provides recommendations to the Centers for Disease Control and Prevention (CDC).
These guidelines are not static; they evolve based on new scientific discoveries, disease prevalence, vaccine efficacy, and public health needs. Adhering to these recommendations is a cornerstone of preventative healthcare, offering protection against a wide array of pathogens that can cause severe illness, disability, or even death.
The continuous review and updating of vaccination schedules reflect a dynamic approach to public health. Researchers are constantly studying vaccine performance, duration of immunity, and the emergence of new strains of viruses and bacteria.
This rigorous scientific process ensures that the guidelines remain relevant and effective in the face of evolving health challenges. For individuals, understanding these updates can mean the difference between robust protection and vulnerability to preventable diseases.
the role of scientific bodies
Scientific bodies play a pivotal role in shaping vaccination guidelines. Their work involves extensive research, clinical trials, and epidemiological studies to assess the safety and effectiveness of vaccines. They also consider factors like vaccine supply, cost-effectiveness, and public acceptance when formulating recommendations.
Data Analysis: Thorough review of clinical trial data and post-market surveillance.
Disease Surveillance: Monitoring disease outbreaks and trends to identify emerging threats.
Expert Consensus: Gathering input from a diverse group of medical and public health professionals.
Public Communication: Translating complex scientific information into accessible guidelines for the public.
The collective effort of these bodies ensures that vaccine recommendations are grounded in robust evidence and tailored to the specific health landscape of the United States.
This scientific foundation builds trust and confidence in the vaccination process, encouraging broader adherence.
In essence, the ongoing development and dissemination of vaccination guidelines are critical for maintaining high levels of population immunity, often referred to as herd immunity.
When a significant portion of the population is vaccinated, it creates a protective barrier that reduces the spread of infectious diseases, safeguarding those who cannot be vaccinated, such as infants, the elderly, or individuals with compromised immune systems.
This collective protection underscores the community-wide benefits of following recommended vaccination schedules.
key updates in adult vaccination schedules
Adult vaccination schedules have seen several important updates in recent years, reflecting new vaccine developments and a deeper understanding of disease prevention across the lifespan.
These changes aim to enhance protection against common and emerging threats, ensuring adults maintain robust immunity as they age. Staying current with these recommendations is essential for personal health and for preventing the spread of diseases within families and workplaces.
One notable area of focus has been on vaccines for respiratory illnesses. The influenza vaccine continues to be an annual recommendation for all adults, with specific formulations sometimes recommended for older adults.
Beyond flu, there have been advancements in vaccines targeting other respiratory pathogens, leading to updated guidance that can significantly reduce morbidity and mortality in older populations and those with underlying health conditions.
new recommendations for respiratory syncytial virus (RSV)
Recent breakthroughs have led to the approval of new vaccines for Respiratory Syncytial Virus (RSV), a common respiratory virus that can cause severe illness in older adults and those with certain medical conditions. The ACIP has issued specific recommendations for these new vaccines.
Target Population: Adults aged 60 years and older.
Risk Factors: Individuals with chronic lung disease, heart disease, or weakened immune systems.
Vaccine Types: Two new RSV vaccines are available, each with specific indications.
Administration: Typically a single dose, often recommended in conjunction with other routine adult vaccinations.
These RSV vaccine recommendations represent a significant step forward in protecting vulnerable adult populations, offering a new layer of defense against a virus that can have serious health consequences.
Healthcare providers are now actively incorporating these vaccines into routine adult care, emphasizing the importance of discussing eligibility with patients.
Furthermore, updates to tetanus, diphtheria, and pertussis (Tdap) vaccinations continue to emphasize the importance of booster shots for adults, especially those who are in close contact with infants.
The shingles vaccine, recommended for adults aged 50 and older, has also seen increased uptake due to its improved efficacy and safety profile. These continuous refinements in adult vaccination schedules highlight a proactive approach to lifelong immunity, ensuring that protection extends well beyond childhood.
childhood immunization: what parents need to know
Childhood immunization remains a cornerstone of public health, protecting infants, children, and adolescents from a range of serious and potentially life-threatening diseases.
The latest vaccination guidelines for children are meticulously crafted to provide optimal protection at critical developmental stages. Parents play a vital role in adhering to these schedules, not only to shield their own children but also to contribute to the overall health and safety of the community.
The CDC’s recommended immunization schedule for children is comprehensive, covering vaccines against diseases such as measles, mumps, rubella (MMR), polio, diphtheria, tetanus, pertussis (DTaP), varicella (chickenpox), and hepatitis B, among others.
Each vaccine is timed to provide protection when children are most vulnerable, ensuring they develop immunity before potential exposure to these illnesses. Pediatricians are key resources for parents, providing guidance and addressing any concerns about the schedule.
navigating the immunization schedule
The childhood immunization schedule can appear complex, but it is designed for maximum effectiveness and safety. Understanding the rationale behind each vaccine and its timing can help parents feel more confident in their decisions.
Birth to 18 Months: Early vaccinations target highly contagious and severe diseases like Hepatitis B, Rotavirus, and DTaP.
18 Months to 6 Years: Boosters for DTaP, MMR, and Varicella, plus initial doses for Hepatitis A and others.
7 to 18 Years: Vaccinations for HPV, meningococcal disease, and Tdap boosters are crucial during adolescence.
Catch-up Schedules: For children who miss doses, specific catch-up schedules are available to ensure they receive full protection.
Open communication with healthcare providers is encouraged to understand the benefits and potential side effects of each vaccine.
Pediatricians can provide personalized advice based on a child’s health history and any specific risk factors. This collaborative approach ensures that every child receives the most appropriate and timely immunizations.
Beyond individual protection, high vaccination rates in childhood are fundamental for achieving herd immunity within schools and communities.
When most children are vaccinated, it significantly reduces the circulation of infectious diseases, protecting infants too young to be vaccinated and children with compromised immune systems.
This collective benefit highlights the profound impact of parental adherence to childhood vaccination guidelines, reinforcing the notion that vaccination is a shared responsibility for public health.
vaccinations for specific populations and travel
Vaccination guidelines extend beyond general adult and childhood schedules to address the unique needs of specific populations and individuals planning international travel. These tailored recommendations are crucial for providing targeted protection against diseases that may pose higher risks due to age, health status, occupation, or geographic exposure. Understanding these specialized guidelines ensures comprehensive immunity for everyone.
For individuals with chronic health conditions, such as diabetes, heart disease, or autoimmune disorders, certain vaccines may be particularly important to prevent severe complications from common infections.
Similarly, healthcare workers, laboratory personnel, and others in high-risk occupations often require additional immunizations to protect themselves and those they serve. These specialized schedules are part of a broader strategy to minimize disease transmission in vulnerable settings.
travel vaccines and international health guidance
International travel can expose individuals to diseases not commonly found in the United States, making travel-specific vaccinations a critical component of pre-travel planning. The CDC provides extensive guidance on required and recommended vaccines based on destination.
Yellow Fever: Required for entry into certain countries in Africa and South America.
Typhoid: Recommended for travelers visiting areas with poor sanitation and food hygiene.
Hepatitis A and B: Often recommended for travelers to regions with high prevalence.
Rabies: Considered for long-term travelers or those engaging in high-risk activities in areas where rabies is common.
Polio: Booster doses may be recommended for travel to polio-endemic regions.
Travelers should consult a healthcare provider or a travel clinic at least 4-6 weeks before their trip to ensure they receive all necessary vaccinations and preventative medications.
This allows sufficient time for vaccines to become effective and for any multi-dose series to be completed. Personalized advice can address specific itineraries, activities, and individual health considerations, ensuring a safe and healthy journey.
Beyond travel, certain medical conditions or treatments, such as organ transplantation or chemotherapy, can necessitate altered vaccination schedules or additional vaccines to compensate for a weakened immune system.
Pregnant women also have specific vaccination recommendations, like the Tdap vaccine, to protect both themselves and their newborns. These examples underscore the dynamic nature of vaccination guidelines, which are constantly adapted to provide the best possible protection for diverse health scenarios and life stages.
addressing common concerns and vaccine hesitancy
Despite the overwhelming scientific evidence supporting vaccine safety and efficacy, concerns and hesitancy persist among some segments of the population.
Addressing these concerns openly and with accurate information is crucial for maintaining high vaccination rates and protecting public health. Healthcare providers play a key role in fostering trust and providing clear, evidence-based answers to patient questions.
Many common concerns revolve around vaccine side effects, the number of vaccines administered, and the perceived risk of vaccine components.
It is important to differentiate between minor, temporary side effects, such as soreness at the injection site or a low-grade fever, and rare, serious adverse events.
Thorough research and transparent communication from health authorities help to put these risks into perspective, demonstrating that the benefits of vaccination far outweigh the potential harms.
debunking myths and promoting informed decisions
Effective communication strategies are essential to counter misinformation and promote informed decision-making regarding vaccinations. This involves providing clear, accessible information from trusted sources.
Vaccine Safety: Emphasizing the rigorous testing and monitoring processes vaccines undergo.
Ingredient Transparency: Explaining vaccine components and their safety profiles.
Disease Risk: Highlighting the severity of vaccine-preventable diseases and their potential complications.
Trusted Sources: Directing individuals to reputable organizations like the CDC, WHO, and local health departments for information.
Healthcare professionals are uniquely positioned to engage in empathetic conversations, addressing individual concerns without judgment.
By providing personalized information and addressing specific fears, they can help individuals make confident decisions about vaccination for themselves and their families.
This approach respects individual autonomy while upholding the collective responsibility for public health.
Furthermore, public health campaigns often utilize various media channels to disseminate accurate information and share personal stories of individuals who have benefited from vaccination.
These narratives can be powerful in illustrating the real-world impact of vaccines and counteracting abstract fears.
Ultimately, building and maintaining trust in vaccines requires ongoing dialogue, transparency, and a commitment to evidence-based communication from all stakeholders, ensuring that vaccination remains a widely accepted and effective public health intervention.
the impact of vaccination on public health outcomes
The profound impact of vaccination on public health outcomes cannot be overstated. Vaccines have been instrumental in eradicating smallpox, dramatically reducing the incidence of polio, and significantly curbing the spread of numerous other infectious diseases that once caused widespread morbidity and mortality.
These achievements highlight vaccination as one of the most successful and cost-effective public health interventions in history, directly contributing to increased life expectancy and improved quality of life globally.
In the United States, the widespread adoption of vaccination programs has transformed the landscape of infectious diseases. Diseases like measles, mumps, and rubella, which were once common childhood scourges, are now rare thanks to high immunization rates.
This success allows healthcare resources to be directed towards other pressing health issues, while also preventing countless hospitalizations, long-term disabilities, and deaths. The economic benefits, from reduced healthcare costs to increased productivity, are equally substantial.

vaccination
measuring success and ongoing challenges
The success of vaccination programs is measured through various public health metrics, including disease incidence, hospitalization rates, and mortality rates. These indicators consistently demonstrate the protective effect of vaccines.
Disease Eradication: The complete elimination of diseases like smallpox.
Incidence Reduction: Significant drops in cases of measles, polio, and diphtheria.
Outbreak Prevention: Preventing large-scale epidemics through herd immunity.
Economic Savings: Billions of dollars saved in healthcare costs and lost productivity.
Despite these successes, ongoing challenges remain, including vaccine hesitancy, the emergence of new pathogens, and ensuring equitable access to vaccines globally.
Public health efforts continuously adapt to these challenges, emphasizing research into new vaccines, improving vaccine delivery systems, and strengthening communication to address public concerns. The commitment to vaccination remains a dynamic and evolving endeavor aimed at securing a healthier future for all.
Ultimately, the story of vaccination is one of continuous progress and collective action. Each vaccine administered not only protects an individual but also reinforces the protective shield around the entire community.
By understanding and adhering to the latest vaccination guidelines, we contribute to a healthier society, safeguarding ourselves and future generations from the burden of preventable infectious diseases. This shared responsibility underscores the enduring value of vaccination as a cornerstone of modern public health.
future trends and innovations in vaccinology
The field of vaccinology is constantly evolving, driven by scientific innovation and the persistent challenge of emerging infectious diseases.
Future trends in vaccination promise even more effective, broader-spectrum, and accessible vaccines, further enhancing our ability to protect public health. Researchers are exploring novel vaccine platforms and delivery methods that could revolutionize how we prevent and control infectious diseases.
One of the most exciting areas of innovation is messenger RNA (mRNA) vaccine technology, which proved its efficacy during the COVID-19 pandemic.
This platform allows for rapid vaccine development and production, offering a flexible approach to respond to new viral threats.
Beyond mRNA, advancements in vector-based vaccines, subunit vaccines, and even universal vaccines designed to protect against multiple strains of a virus are on the horizon, promising more comprehensive and durable immunity.
personalized vaccines and enhanced delivery systems
Future vaccinology is also moving towards more personalized approaches, tailoring vaccines to individual genetic profiles or specific immune responses. This could lead to more potent and targeted protection.
Personalized Medicine: Vaccines designed based on an individual’s immune system characteristics.
Microneedle Patches: Painless, self-administered patches that deliver vaccines through tiny needles, eliminating the need for traditional injections.
Adjuvant Development: New adjuvants that enhance immune responses, allowing for lower vaccine doses or fewer injections.
Therapeutic Vaccines: Vaccines designed to treat existing conditions, such as cancer or chronic infections, rather than just preventing them.
These innovations hold the potential to overcome current vaccination challenges, such as cold chain requirements for vaccine storage, vaccine hesitancy due to needle phobia, and the need for rapid responses to pandemics.
The integration of artificial intelligence and machine learning in vaccine design is also accelerating the discovery process, allowing scientists to identify promising vaccine candidates more efficiently.
The ongoing commitment to research and development in vaccinology reflects a global understanding that vaccines are a critical tool in the fight against infectious diseases.
As these trends mature, we can anticipate a future where vaccine protection is more robust, more accessible, and more finely tuned to individual and community needs, continuously safeguarding public health against both known and unforeseen threats.
This relentless pursuit of innovation ensures that the benefits of vaccination will continue to grow, offering hope for a world less burdened by infectious illness.
| Key Aspect | Brief Description |
|---|---|
| Evolving Guidelines | Vaccination recommendations are regularly updated by scientific bodies like ACIP/CDC based on new data and disease trends. |
| Adult Updates | Important changes include new RSV vaccines and enhanced guidance for flu, Tdap, and shingles for various age groups. |
| Childhood Protection | Comprehensive schedules protect against critical childhood diseases, crucial for individual and herd immunity. |
| Future Innovations | mRNA technology, personalized vaccines, and enhanced delivery systems promise more effective and accessible immunizations. |
frequently asked questions about vaccinations
Vaccination guidelines are updated regularly to reflect new scientific research, the emergence of new diseases or strains, changes in vaccine efficacy, and evolving public health needs. This ensures the recommendations remain effective and provide optimal protection for the population.
Herd immunity occurs when a large percentage of a community is vaccinated, making it difficult for infectious diseases to spread. This protects vulnerable individuals who cannot be vaccinated, such as infants or those with compromised immune systems, by reducing their exposure risk.
Yes, several vaccines are recommended and safe for pregnant women, such as the flu shot and Tdap vaccine. These not only protect the mother but also provide crucial antibodies to the developing baby, offering protection in the first few months of life.
Reliable information on vaccination schedules can be found on the websites of the Centers for Disease Control and Prevention (CDC), the World Health Organization (WHO), and your local public health department. Your healthcare provider is also an excellent source of personalized guidance.
If you or your child missed a vaccine dose, consult your healthcare provider immediately. They can provide a catch-up schedule to ensure you receive the necessary protection without having to restart the entire vaccination series.
conclusion
The latest vaccination guidelines in the USA serve as a vital framework for safeguarding individual health and fostering robust community immunity.
By staying informed about these evolving recommendations, from childhood immunizations to adult boosters and specialized travel vaccines, we actively participate in preventing the spread of infectious diseases.
The continuous dedication to scientific research and public health communication ensures that vaccines remain one of our most effective tools in achieving a healthier, more resilient society. Embracing these guidelines is a shared responsibility that protects us all.





