New Cancer Screening Advances: What to Expect in 2026

 The landscape of cancer detection is on the cusp of a monumental shift, promising more precise and less invasive methods for early diagnosis.
The landscape of cancer detection is on the cusp of a monumental shift, promising more precise and less invasive methods for early diagnosis.
As we look towards 2026, the discussion around New Advances in Cancer Screening: What to Expect in 2026 is no longer theoretical, but a tangible reality for millions. This evolution brings hope for improved patient outcomes and a proactive approach to health.
The Dawn of Non-Invasive Diagnostics
The pursuit of less invasive yet highly accurate cancer screening methods has been a cornerstone of medical research for decades.
By 2026, we anticipate a significant leap in this area, moving beyond traditional biopsies and imaging techniques to embrace technologies that can detect cancer with minimal discomfort and risk to the patient.
This shift is not merely about convenience; it’s about making screening accessible and appealing to a broader population, ultimately saving more lives through earlier intervention.
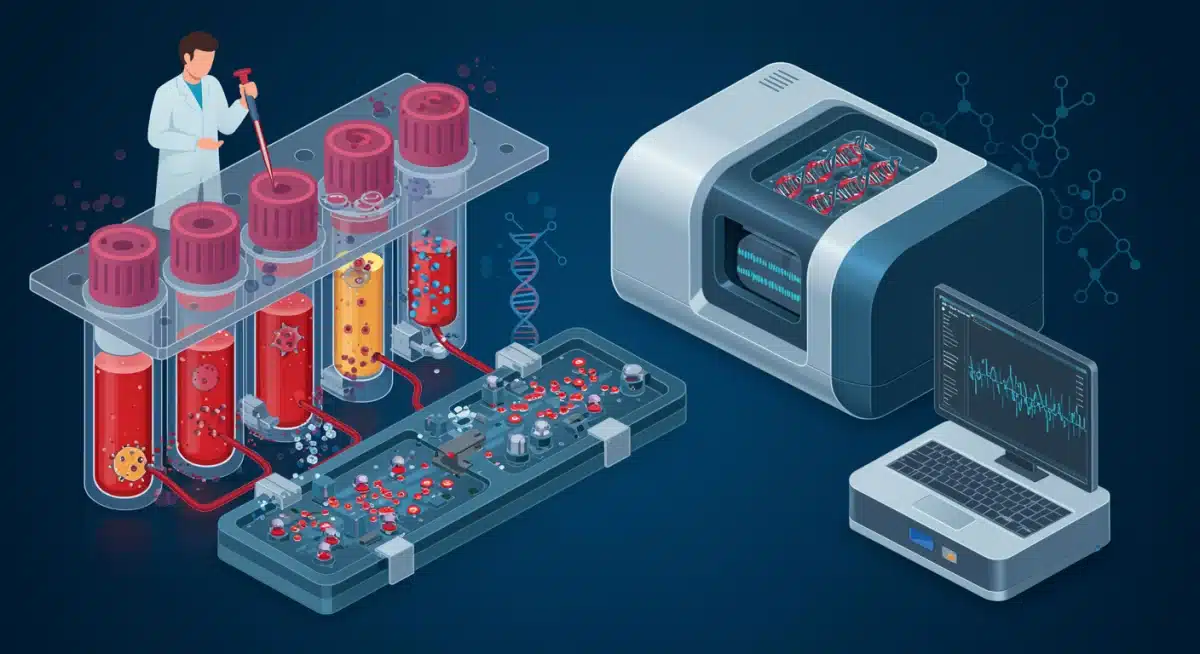
One of the most exciting frontiers is the development of liquid biopsies, which promise to revolutionize how we approach cancer detection. These tests analyze biological fluids, primarily blood, for markers indicative of cancer.
The potential for these methods to detect cancer at its earliest stages, even before symptoms appear, is immense, offering a paradigm shift in preventive healthcare.
Liquid Biopsies: A Game Changer
Liquid biopsies represent a significant advancement, capable of identifying circulating tumor DNA (ctDNA), circulating tumor cells (CTCs), and other biomarkers released by tumors into the bloodstream.
This non-invasive approach reduces the need for surgical biopsies, which can be painful, risky, and sometimes inconclusive.
Early Detection: Liquid biopsies can detect cancer signals much earlier than conventional methods.
Monitoring Treatment: They offer a way to monitor treatment effectiveness and detect recurrence in real-time.
Personalized Medicine: These tests can help tailor treatments by identifying specific genetic mutations in tumors.
The integration of liquid biopsies into routine screening protocols by 2026 could mean that a simple blood test might become a primary tool for detecting various cancers, making screening more comfortable and widespread.
This technology holds particular promise for cancers that are currently difficult to screen for, such as pancreatic or ovarian cancer, where early detection dramatically improves survival rates.
In essence, the move towards non-invasive diagnostics is about empowering individuals with accessible tools for proactive health management.
The convenience and safety of these methods are expected to increase compliance with screening recommendations, thereby improving public health outcomes on a national scale. The advancements in this field are backed by extensive research and clinical trials, ensuring their reliability and efficacy.
AI and Machine Learning: Enhancing Diagnostic Accuracy
Artificial intelligence (AI) and machine learning (ML) are no longer futuristic concepts in healthcare; they are rapidly becoming indispensable tools in cancer diagnostics. By 2026, their role in enhancing the accuracy and efficiency of cancer screening is expected to be profoundly integrated across various medical disciplines.
These technologies possess the capacity to analyze vast amounts of data, identifying patterns and anomalies that might be imperceptible to the human eye, thereby augmenting the diagnostic capabilities of healthcare professionals.
The application of AI in medical imaging, pathology, and even genetic sequencing is set to transform how quickly and accurately cancers are detected. This integration means earlier diagnoses, more precise treatment planning, and ultimately, better chances of survival for patients.
Smarter Image Analysis
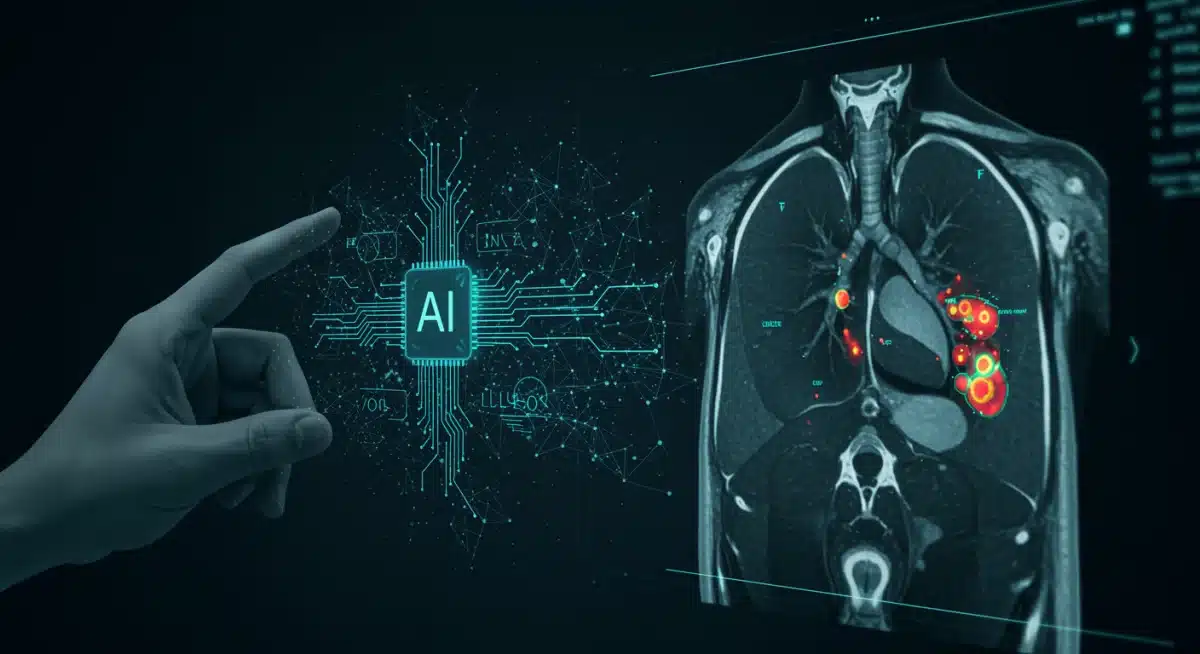
AI algorithms are being trained on millions of medical images, allowing them to detect subtle signs of cancer with remarkable precision. This includes mammograms, CT scans, MRIs, and pathology slides.
Improved Detection Rates: AI can identify cancerous lesions that might be missed by human interpretation alone.
Reduced False Positives: By refining diagnostic criteria, AI helps decrease the number of unnecessary follow-up procedures.
Faster Diagnosis: Automated analysis speeds up the diagnostic process, reducing patient anxiety and wait times.
Beyond imaging, machine learning is also being applied to analyze complex genomic data, identifying genetic predispositions to cancer and predicting treatment responses. This level of personalized insight is crucial for the future of precision oncology.
The ability of AI to learn and adapt from new data ensures that its diagnostic capabilities will continually improve, making it an increasingly valuable asset in the fight against cancer. This ongoing evolution promises to bring a level of accuracy and speed to diagnostics previously unimaginable, making healthcare more proactive and personalized.
The synergy between human expertise and AI-powered tools will define the future of cancer diagnostics. While AI can process data at an unparalleled speed, the critical thinking and empathetic approach of human clinicians remain irreplaceable.
Together, they form a formidable team in the quest for early and accurate cancer detection, ensuring that patients receive the best possible care. The advancements in AI are not about replacing doctors but empowering them with superior tools to make informed decisions.
Precision Medicine and Personalized Screening Protocols
The move towards precision medicine is fundamentally reshaping how cancer screening is approached, transitioning from a one-size-fits-all model to highly individualized protocols.
By 2026, personalized screening will be a cornerstone of cancer prevention, leveraging an individual’s genetic makeup, lifestyle, and medical history to determine the most effective and appropriate screening schedule and methods.
This tailored approach aims to maximize the benefits of screening while minimizing potential harms, such as over-diagnosis or unnecessary procedures.
Understanding an individual’s unique risk factors allows healthcare providers to implement screening strategies that are far more effective than generic guidelines. This means that some individuals might require more frequent or intensive screening, while others might benefit from less aggressive approaches, all based on their specific risk profile.
Genetic Testing and Risk Assessment
Genetic testing plays a pivotal role in personalizing cancer screening. Identifying inherited mutations that increase cancer risk, such as BRCA1/2 for breast and ovarian cancer, allows for targeted early detection strategies.
Familial Risk Identification: Pinpointing individuals with a higher genetic predisposition to certain cancers.
Proactive Screening Plans: Developing customized screening schedules, potentially starting earlier or using more advanced techniques.
Preventive Measures: Informing decisions about risk-reducing medications or prophylactic surgeries.
The integration of comprehensive risk assessment, including both genetic and lifestyle factors, will enable the creation of highly personalized health roadmaps. These roadmaps will guide patients and their physicians in making informed decisions about screening frequency, types of tests, and preventive interventions.
The goal is to detect cancer when it is most treatable, often before it has even developed into an invasive disease. This proactive and individualized approach signifies a major shift in how healthcare is delivered, moving towards truly patient-centered models. The ability to predict and prevent, rather than merely react, is a powerful development in modern medicine.
Furthermore, lifestyle analytics, combined with genetic insights, will offer a holistic view of an individual’s cancer risk. Factors such as diet, exercise, environmental exposures, and even microbiome composition are increasingly being recognized for their role in cancer development.
Incorporating these elements into personalized screening protocols makes the approach even more comprehensive and effective, ensuring that all relevant risk factors are considered.
This comprehensive data integration will enable healthcare providers to offer truly bespoke screening advice, optimizing both the efficiency and efficacy of cancer detection efforts.
Advanced Imaging Techniques: Sharper Views, Earlier Detection
While liquid biopsies and AI are generating considerable excitement, traditional imaging techniques are also undergoing significant advancements, promising even sharper views of internal structures and earlier detection of cancerous lesions.
By 2026, we can expect to see widespread adoption of next-generation imaging technologies that offer higher resolution, better contrast, and more functional information about tissues. These innovations are critical for visualizing small tumors and accurately staging the disease.
These advanced imaging modalities are not just about seeing more clearly; they are about providing a deeper understanding of tumor biology. This includes assessing blood flow, metabolic activity, and cellular density, all of which can provide valuable clues about the presence and aggressiveness of cancer.
Enhanced MRI and PET Scans
Magnetic Resonance Imaging (MRI) and Positron Emission Tomography (PET) scans are continually evolving, offering unparalleled insights into the body’s internal workings.
Diffusion-Weighted MRI: Improved ability to detect tiny tumors by measuring water molecule movement in tissues.
Hybrid PET/MRI Systems: Combining the anatomical detail of MRI with the metabolic information of PET for comprehensive imaging.
Molecular Imaging: Using targeted tracers to highlight specific cancer cells, even at microscopic levels.
Beyond these established modalities, emerging technologies such as photoacoustic imaging and optical coherence tomography are showing promise for detecting superficial cancers with high precision. These techniques offer non-ionizing radiation alternatives, making them safer for repeated use and for younger patients.
The continuous refinement of imaging technology is crucial for identifying cancers that might otherwise go undetected until they are more advanced, emphasizing the importance of ongoing research and development in this field. The clearer the image, the earlier and more accurately a diagnosis can be made, leading to more successful treatment outcomes.
Furthermore, the integration of AI with these advanced imaging techniques further amplifies their diagnostic power. AI algorithms can analyze complex imaging data faster and more accurately than human radiologists, identifying subtle changes that might indicate early-stage cancer.
This symbiotic relationship between advanced hardware and intelligent software is propelling cancer screening into an era of unprecedented precision and efficacy, ensuring that no stone is left unturned in the pursuit of early detection. The combination of these forces is creating a diagnostic environment where even the most elusive cancers have fewer places to hide.
Multi-Cancer Early Detection (MCED) Tests
One of the most anticipated innovations by 2026 is the widespread availability and refinement of multi-cancer early detection (MCED) tests. These groundbreaking tests aim to detect multiple types of cancer from a single blood sample, offering a transformative approach to population-level screening.
Unlike traditional screening methods that are often limited to one or two specific cancer types (e.g., mammography for breast cancer, colonoscopy for colorectal cancer), MCED tests seek to provide a comprehensive overview of cancer risk across various organs.
The promise of MCED tests lies in their potential to address the challenge of cancers for which no routine screening currently exists, such as ovarian, pancreatic, and esophageal cancers. Early detection for these aggressive cancers can significantly improve survival rates, making MCED tests a critical tool in the ongoing battle against cancer.
How MCED Tests Work
MCED tests typically look for cancer signals by analyzing circulating tumor DNA (ctDNA) fragments or other biomarkers in the blood. These fragments carry genetic or epigenetic alterations characteristic of cancer, allowing for the identification of a potential tumor and even its tissue of origin.
Broad Spectrum Detection: Ability to screen for dozens of cancer types simultaneously.
Non-Invasive: Requires only a blood draw, making it highly accessible and patient-friendly.
Complementary to Existing Screens: Designed to complement, not replace, established single-cancer screening methods.
The development and validation of MCED tests involve rigorous clinical trials to ensure their accuracy, sensitivity, and specificity. While these tests are not yet perfect, rapid advancements in genomics and bioinformatics are quickly improving their performance.
The goal is to achieve a level of reliability that makes them suitable for widespread adoption in routine health check-ups, potentially becoming a standard part of annual physicals for adults over a certain age.
This could drastically increase the number of cancers caught at an early, treatable stage. The impact on public health could be immense, shifting the paradigm from late-stage diagnosis to early intervention, thus reducing the burden of advanced cancer.
Moreover, the economic implications of MCED tests are substantial. By detecting cancers earlier, the costs associated with advanced treatment, long-term care, and lost productivity can be significantly reduced. This makes MCED tests not only a medical breakthrough but also a financially sound investment in public health.
As these tests become more refined and affordable, their integration into healthcare systems will represent a monumental step forward in cancer prevention and management, ensuring a healthier future for communities across the nation.
The ongoing research and development in this area are critical to realizing the full potential of these revolutionary diagnostic tools.
Implementation Challenges and Ethical Considerations
While the promise of new cancer screening advances by 2026 is immense, their successful implementation will undoubtedly face a range of challenges and ethical considerations. Integrating these sophisticated technologies into existing healthcare infrastructures requires careful planning, significant investment, and robust regulatory frameworks.
It’s not enough to simply develop new tests; we must ensure they are accessible, affordable, and equitably distributed across all demographics.
One primary challenge lies in the cost-effectiveness of these new technologies. Advanced diagnostics often come with a high price tag, raising questions about insurance coverage, patient out-of-pocket expenses, and the overall sustainability of healthcare systems.
Ensuring that these innovations do not exacerbate existing health disparities will be a critical task for policymakers and healthcare providers alike. The benefits of early detection should be available to everyone, regardless of their socioeconomic status.
Navigating the Ethical Landscape
The introduction of highly sensitive screening tests also brings forth a host of ethical dilemmas that need careful consideration.
False Positives and Over-diagnosis: The risk of identifying benign conditions as cancerous, leading to unnecessary anxiety and invasive follow-up procedures.
Data Privacy: Protecting sensitive genetic and health information generated by personalized screening protocols.
Equity of Access: Ensuring that technological advancements do not create a two-tiered healthcare system where only the affluent benefit.
Moreover, the psychological impact of screening, particularly for MCED tests that might yield uncertain results or detect conditions with unknown clinical significance, needs to be thoroughly addressed. Patients will require clear communication and robust support systems to navigate these complexities.
The balance between early detection and avoiding undue patient burden is a delicate one that demands ongoing dialogue between medical professionals, ethicists, and the public.
As these technologies become more prevalent, the ethical frameworks governing their use must evolve in parallel, ensuring that patient well-being remains at the forefront of all decisions.
This includes informed consent processes that clearly outline the potential benefits and risks of new screening methods.
Addressing these challenges will require a concerted effort from all stakeholders, including government bodies, healthcare organizations, research institutions, and patient advocacy groups.
Developing clear guidelines for the use of new screening technologies, establishing fair pricing models, and investing in public education campaigns will be crucial for successful adoption.
Only through a holistic and thoughtful approach can we fully realize the potential of these new advances in cancer screening, ensuring they serve to improve health outcomes for all. This collaborative effort will shape the future of cancer prevention, making it more effective and equitable for everyone.
| Key Advance | Brief Description |
|---|---|
| Liquid Biopsies | Non-invasive blood tests detecting cancer DNA or cells for early diagnosis and monitoring. |
| AI-Powered Diagnostics | Artificial intelligence analyzing medical images and data for enhanced accuracy and speed in detection. |
| Personalized Screening | Tailoring screening protocols based on individual genetic, lifestyle, and medical risk factors. |
| MCED Tests | Single blood tests designed to detect multiple types of cancer simultaneously, expanding early detection. |
Frequently asked questions about cancer screening in 2026
A liquid biopsy is a non-invasive blood test that detects cancer markers like ctDNA. By 2026, it’s expected to become a widespread tool for early cancer detection, disease monitoring, and guiding treatment decisions, offering a less invasive alternative to traditional biopsies and improving accessibility for patients.
AI will significantly enhance cancer screening by analyzing medical images and complex data with greater speed and precision than humans. It can identify subtle anomalies, reduce false positives, and accelerate diagnosis, particularly in fields like radiology and pathology, leading to earlier and more reliable detection of cancerous growths.
Personalized screening means tailored cancer detection plans based on an individual’s unique genetic profile, lifestyle, and medical history. By 2026, this approach will optimize screening frequency and methods, ensuring more effective and less burdensome tests for each person, moving away from generic guidelines to precision prevention strategies.
No, MCED tests are designed to complement, not replace, existing single-cancer screenings like mammograms or colonoscopies. By 2026, they are expected to offer a broad initial screen for many cancers currently lacking routine tests, identifying potential issues that can then be investigated with more specific, established diagnostic methods.
Key ethical considerations include managing false positives and over-diagnosis, safeguarding patient data privacy, and ensuring equitable access to these advanced technologies. Striking a balance between early detection benefits and potential patient anxiety or healthcare disparities will be crucial as these innovations become more widespread by 2026.
Conclusion
The rapid evolution of cancer screening technologies promises a future where early detection is not just a hope, but a widespread reality. As we approach 2026, the integration of liquid biopsies, AI-driven diagnostics, personalized screening protocols, and multi-cancer early detection tests is poised to revolutionize how we approach cancer prevention and management.
These advancements offer the potential for more accurate, less invasive, and highly individualized screening experiences, ultimately leading to improved patient outcomes and a significant reduction in cancer-related mortality.
While challenges related to implementation, cost, and ethics remain, the collective efforts of researchers, healthcare providers, and policymakers are paving the way for a healthier future, where cancer is detected earlier, treated more effectively, and its devastating impact is significantly lessened for communities across the United States.





